Penicillin allergy is the most frequently reported drug allergy worldwide, affecting approximately 10% of the general population. Despite this high prevalence, clinical evidence demonstrates that nearly 90% of individuals labeled as penicillin-allergic do not have a true IgE-mediated hypersensitivity reaction. This discrepancy highlights a major issue in modern healthcare: the widespread misclassification and persistence of inaccurate antibiotic allergy labels.
Incorrect documentation of penicillin allergy has significant clinical and economic consequences, particularly in outpatient care settings where beta-lactam antibiotics remain the first-line treatment for many common infections in both adults and pediatric populations. When patients are incorrectly labeled as allergic, clinicians often resort to alternative or broad-spectrum antibiotics. This practice is associated with increased risks, including adverse drug reactions, higher healthcare costs, suboptimal clinical outcomes, and a greater likelihood of developing antimicrobial resistance.
In addition, inappropriate antibiotic selection contributes to complications such as Clostridioides difficile infection, which is strongly linked to the use of broad-spectrum agents. Although much of the available data originates from inpatient settings, similar patterns are observed in outpatient care, where patients with documented penicillin allergies tend to receive more antibiotics, incur higher treatment costs, and utilize more healthcare resources.
A critical factor underlying this issue is the misdiagnosis of penicillin allergy. Many reported reactions are either non-allergic adverse effects or hypersensitivity reactions that diminish over time. Studies indicate that approximately 80% of patients with a true penicillin allergy lose sensitivity after ten years. Despite this, both patients and healthcare providers often remain unaware that re-evaluation is possible.
This gap in knowledge presents an important opportunity for improved outpatient management through structured penicillin allergy assessment and the use of penicillin skin testing (PST). These approaches enable accurate identification of true allergies, facilitate safe de-labeling of patients, and support appropriate antibiotic prescribing.
Penicillin Allergy Assessment in Clinical Practice
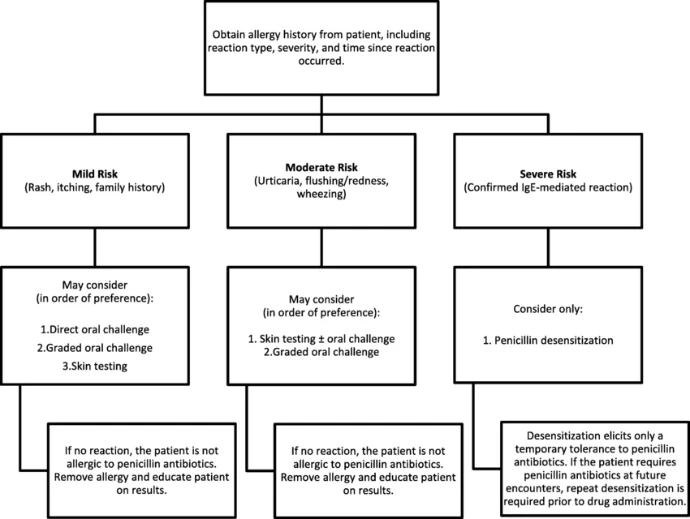
Effective evaluation of a reported penicillin allergy begins with a comprehensive and structured patient interview. This assessment is essential for determining the likelihood of a true allergic reaction and guiding further diagnostic or therapeutic decisions.
Key components of the assessment include:
- Detailed description of the reported reaction
- Timing of symptom onset relative to drug exposure
- Classification of reaction type (IgE-mediated vs non-IgE-mediated)
- Severity and clinical manifestations
- History of exposure to other beta-lactam antibiotics
- Previous allergy testing or medical evaluations
Accurate characterization of the reaction is particularly important, as many patients confuse mild adverse effects with true allergic responses. For example, gastrointestinal intolerance or non-specific rashes are often misinterpreted as allergies, while more severe reactions such as urticaria, angioedema, or anaphylaxis indicate a higher risk profile.
In clinical practice, patients may have difficulty recalling details of past reactions, especially if they occurred many years earlier. Therefore, healthcare providers should use a combination of open-ended and targeted questions to improve the accuracy of the assessment. Reviewing pharmacy records and medication history can also provide valuable information regarding prior tolerance to beta-lactam antibiotics.
Another critical aspect is understanding cross-reactivity among beta-lactam antibiotics. Structural similarities, particularly in the R1 side chain, influence the likelihood of cross-reactivity between penicillins, cephalosporins, and other related agents. Recognizing these patterns allows clinicians to safely prescribe alternative antibiotics when appropriate.
Role of Penicillin Skin Testing (PST)
Penicillin skin testing is a validated and reliable diagnostic tool used to identify IgE-mediated hypersensitivity reactions. It is considered safe and effective when performed under controlled conditions and can significantly reduce unnecessary antibiotic avoidance.
Traditionally, PST has been conducted in specialized allergy clinics; however, its application in outpatient settings is expanding. The procedure typically involves:
- Skin prick testing using major and minor penicillin determinants
- Intradermal testing with controlled antigen concentrations
- Observation for immediate hypersensitivity reactions
- Optional oral challenge with amoxicillin if skin tests are negative
A negative PST result, particularly when followed by an oral challenge, has a high negative predictive value, approaching 100%. This allows clinicians to confidently remove the penicillin allergy label and reintroduce beta-lactam antibiotics when clinically indicated.
Despite its benefits, PST remains underutilized due to barriers such as limited access to testing centers, lack of clinician awareness, and logistical constraints.
Expanding the Role of Pharmacists
Pharmacists are uniquely positioned to play a central role in outpatient penicillin allergy management. Their expertise in pharmacotherapy, accessibility to patients, and integration within healthcare teams make them ideal candidates for conducting allergy assessments and facilitating PST services.
Potential pharmacist contributions include:
- Performing structured allergy interviews
- Identifying patients eligible for PST
- Providing patient and provider education
- Coordinating referrals to allergy specialists
- Participating in or directly conducting PST (where permitted)
- Ensuring accurate documentation in electronic medical records
Referral Strategies and Target Populations
Proactive referral for penicillin skin testing is a key strategy to reduce the burden of inaccurate allergy labels. Outpatient populations that may benefit from targeted referral include:
- Patients with frequent antibiotic use
- Individuals in long-term care facilities
- Pediatric patients with recurrent infections
- Emergency and urgent care patients
- Preoperative patients requiring antibiotic prophylaxis
Cost, Time, and Resource Considerations
Implementation of PST in outpatient settings requires careful consideration of time, cost, and resource allocation. The total duration of the procedure can range from 45 to 120 minutes, depending on the complexity of the assessment and testing protocol.
Costs associated with PST include:
- Testing reagents and supplies
- Personnel time
- Facility and operational expenses
Despite these upfront costs, long-term economic benefits are significant. These include reduced antibiotic expenditures, decreased hospital admissions, shorter lengths of stay, and lower rates of healthcare-associated infections.
Additionally, PST is a reimbursable procedure in many healthcare systems, further supporting its integration into outpatient practice.Commencez à écrire ici ...
Penicillin allergy assessment and skin testing are integral components of antimicrobial stewardship programs. By reducing unnecessary use of broad-spectrum antibiotics, these interventions help limit the development of antimicrobial resistance and improve overall healthcare quality.
Outpatient settings provide a valuable opportunity to implement these strategies on a large scale. Through coordinated efforts involving pharmacists, physicians, and healthcare organizations, it is possible to significantly reduce the burden of inaccurate penicillin allergy labeling.
Penicillin allergy mislabeling is a widespread and clinically significant issue that negatively impacts antibiotic prescribing practices and patient outcomes. The integration of structured allergy assessment and penicillin skin testing in outpatient settings offers a practical and effective solution.
Pharmacists play a critical role in this process, contributing to patient education, clinical assessment, and antimicrobial stewardship efforts. Expanding access to PST, improving documentation practices, and Enhance education for both patients and clinicians are essential steps toward optimizing antibiotic use.
A comprehensive, multidisciplinary approach is required to address this challenge and ensure that patients receive safe, effective, and evidence-based treatment for infectious diseases.